Mr Morritt regularly performs prominent ear correction surgery (otoplasty or pinnaplasty, ear pinning) at the Spire Claremont Hospital and Thornbury Hospital in Sheffield. He aims to produce natural results from ear pinning surgery and uses a modern technique (the ‘Ear stitch’ technique) where permanent sutures are placed in the ear cartilage to hold the ear in position. In contrast to older techniques, this technique is less invasive and recovery is therefore faster.
Features of prominent ears
There are a wide range of different ear shapes that are considered within the ‘normal’ range for humans. Most humans have minor differences between their right and left ears (asymmetry). Sometimes one or both ears may be prominent. Ear prominence can affect the whole ear or only the top or bottom of the ear. Prominent ears frequently have a poorly defined ear fold (the antehelical fold). In some patients the angle (conchomastoid angle) between the ear and the skull is too big and this causes the ears to appear prominent. In other patients with prominent ears the prominence is caused by a deep conchal bowl. For some patients the ear axis (ear lean) is such that the upper part of the ear is positioned more outward than the lower, giving an appearance of prominence.
Prominent ear correction – the procedure
Mr Morritt most frequently performs prominent ear correction surgery under local anaesthetic (with the patient awake). The advantage of this is that the patient can check the appearance of the ears before during surgery and minor adjustments to shape and position can be made where required. Some patients are scared of needles and in those instances the surgery is performed with intravenous (through a drip) sedation or General anaesthesia (patient is asleep). The surgery is performed as a daycare meaning the patient can go home the same day that surgery takes place. Surgery is most frequently performed to correct both ears (bilateral) but sometimes patients only seek correction of one ear (unilateral).
Local anaesthetic is injected around the ear and into the ear itself. A cut is made behind the ear and a small amount of skin removed. Internal permanent stitches are inserted to improve the ear fold definition (antehelical fold) and reduce ear prominence. Additional stitches are sometimes also placed in the bowl of the ear (conchal bowl) to pull it closer to the skull (these are called concho-mastoid sutures). The position is checked with the patient and if any minor adjustments are desired they are performed. The ear is stitched closed and head band applied. Surgery usually takes between 35 mins (one ear) and 1hr 10 min (both ears). The patient usually goes home on the day of surgery then returns after 1 week for stitch removal. Mr Morritt advises patients to wear the head band 24 hrs a day for 1 week and then requests that the band is worn at night for a further 3 months. After surgery, Mr Morritt advises patients to avoid any face mask that hooks around the ears as this can pull on the ears making them more prominent.
Before and after prominent ear correction surgery
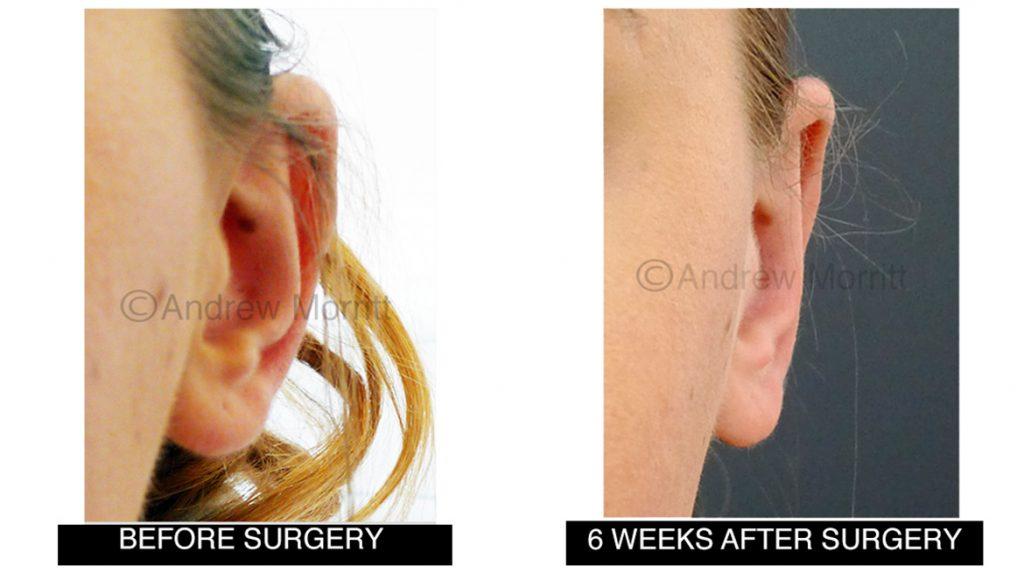
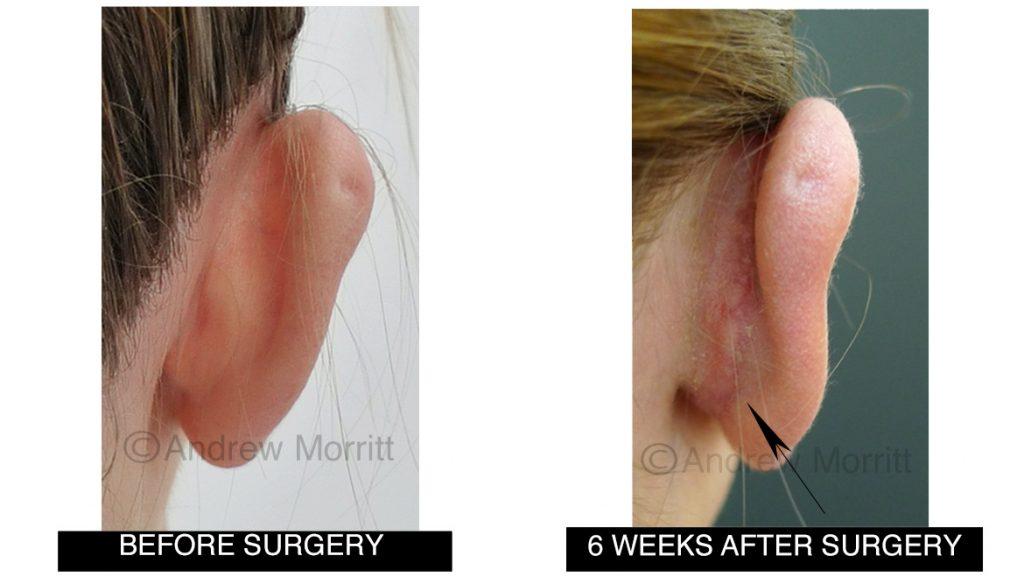
Case 1. Before and after prominent ear correction surgery (pinnaplasty). Internal stitches have been used to bring the top and middle of the ear inward and also to pull the whole ear closer to the skull. The arrow shows the scar which is already difficult to see even at this relatively early stage in healing following otoplasty.
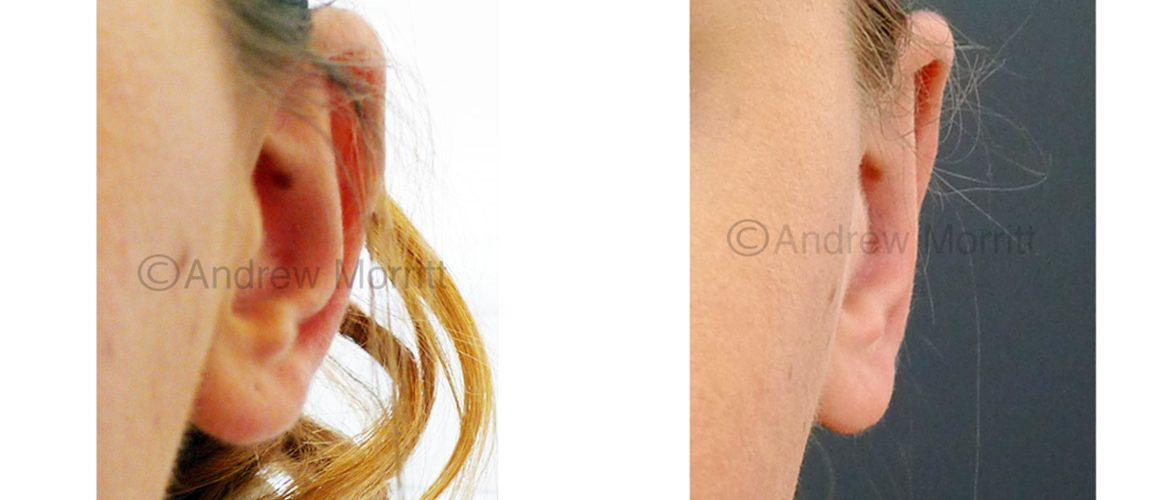
Case 2. Photos showing appearances before and after prominent ear correction surgery (otoplasty) in a lady in her 20’s. Internal stitches have been used to bring the top and middle of the ear inward and give definition to the antehelical fold. It was great to hear how the ear pinning surgery improved this lady’s confidence.
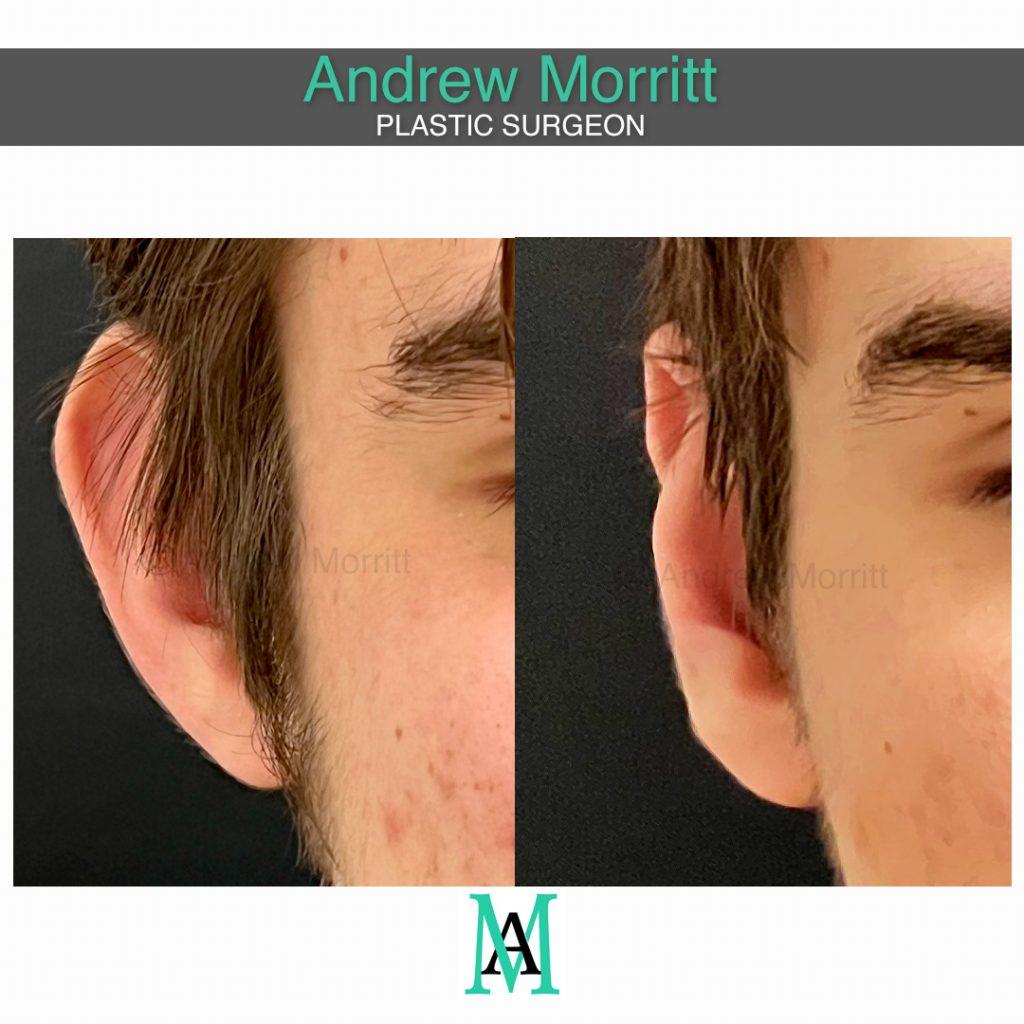
Case 3. Photos showing appearances before and after prominent ear correction surgery (ear pinning) for a man in his early 20s. Internal sutures have been used in the ear cartilage to increase the definition of the antehelical fold, making the ears less prominent whilst maintaining a natural look.
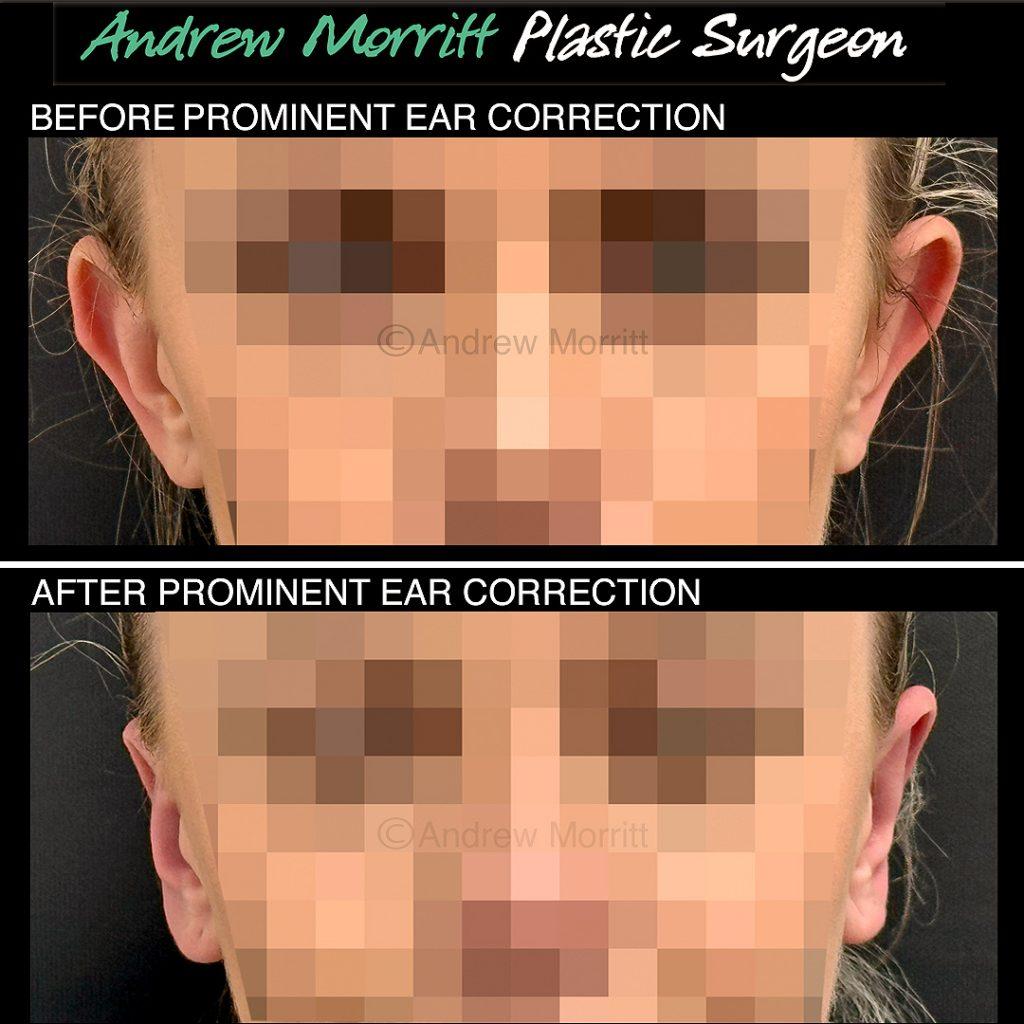
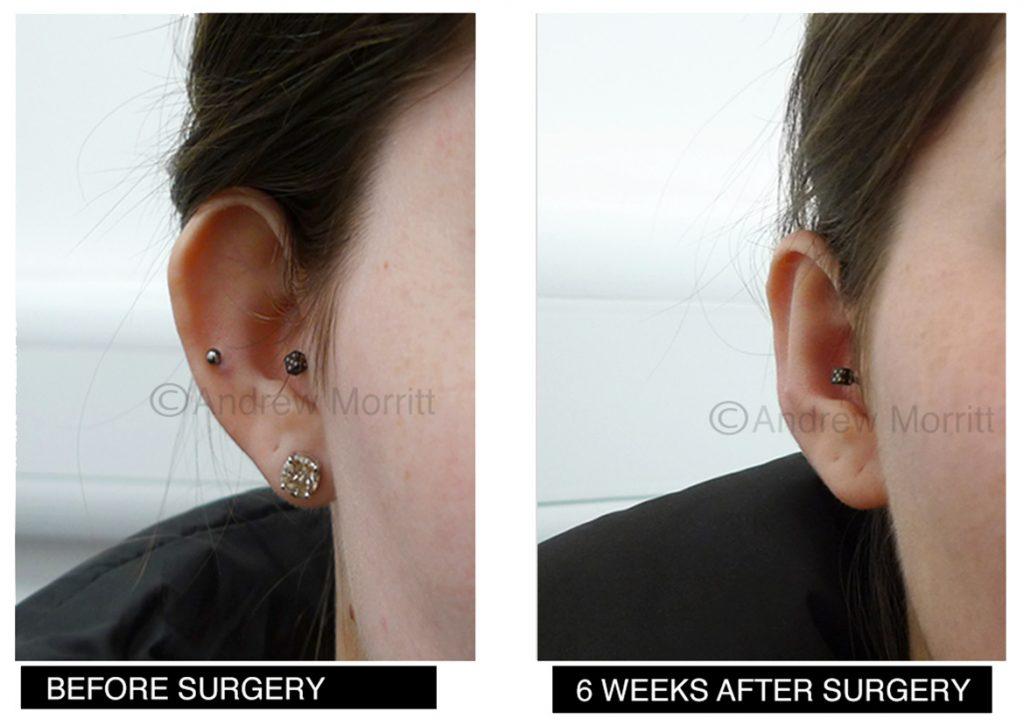
Case 4. Photos showing appearances before and after prominent ear correction surgery with the ‘ear stitch’ technique. Sutures have been inserted to give more definition to the antehelical fold which in turn reduces ear prominence. This lady’s skull shape slopes meaning that it is more prominent in the upper part than the lower part which limits the amount that the prominence in the upper part of the ear can be reduced by ear pinning. Thanks to my kind patient for giving permission to show these results.
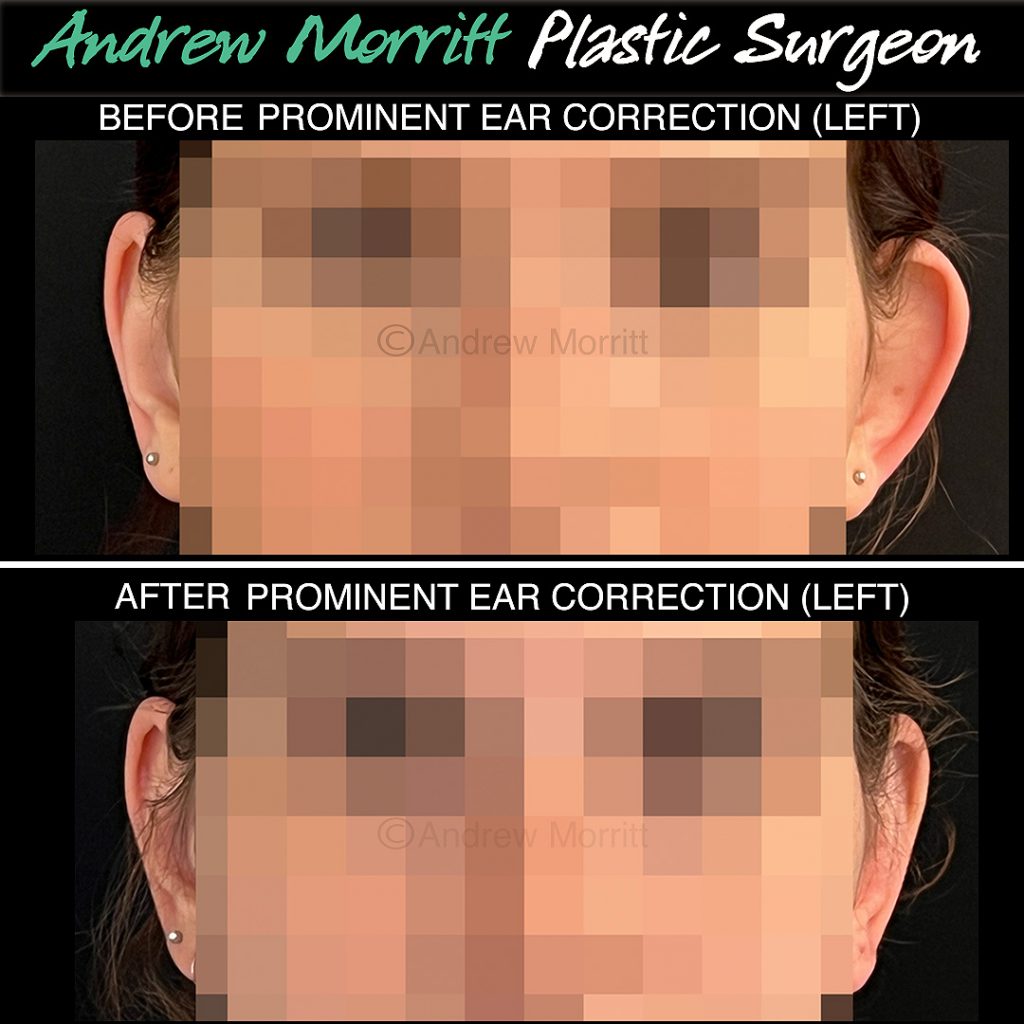
Case 5. Before and after left prominent ear correction surgery. The left ear has been pinned back using internal stitches in the ante helical fold. This has improved the symmetry between the patients ears. Thanks to my patient for giving permission to show these photos from her otoplasty.
Risks of ear correction surgery
Mr Morritt’s prominent ear correction technique is much less invasive than traditional prominent ear correction techniques such as cartilage scoring (“Chongchet”) which means that complications are rare and recovery from surgery is quicker.
Poor scar – scars are generally ultimately thin, pale and flat but can rarely become permanently thick, red and raised.
Bleeding – ears have a very good blood supply and bleeding after surgery can occur. Patients must not undertake any physical activity during the first week after surgery and are advised to avoid NSAIDs e.g. neurofen or ibuprofen. If bleeding is significant a return to the operating theatre may be necessary. Patients can reduce the risk of bleeding by sleeping propped up in bed in the first few days immediately after surgery.
Infection – rare. Skin infection usually requires a course of oral antibiotics. Severe infections can affect the cartilage (chondritis) which is a significant problem though thankfully rare and may lead to long term changes in ear shape.
Asymmetry – no ears are identical before or after surgery. It is therefore likely that after surgery patients will still notice differences between their ears.
Recurrence of ear prominence – it is possible for the ears to become prominent again after surgery. The chance of this is reduced when patients wear the head bandage as recommended and avoid contact sports. The stitches holding the ear in it’s new position are relatively thin and can sometimes snap if subjected to trauma or may tear through the ear cartilage itself meaning that the cartilage is no longer held in place.
Numbness of skin – this is common behind the ear. Usually improves with time but may be permanent.
Chronic ear pain – this is relatively common in the weeks after surgery but usually settles with time. Rarely, patient’s ears may be so sensitive that they can’t lie on that side when in bed. Ears may be painful in cold weather.
Visible stitches – Very rare. Sometimes the internal sutures (most frequently green in colour) can be seen on close inspection in patients with very pale, thin skin. Very rarely the sutures can ulcerate/erode through the skin or granulomas can form.
Skin necrosis – a rare complication.
Wound healing problems – as with all operations it is possible to have wound healing problems after prominent ear correction surgery. Rarely, sutures can ulcerate through the scar which may necessitate further surgery to replace the suture.
Unhappiness with the cosmetic result – some factors that cause ears to appear prominent cannot be altered with surgery – these include cases where the patient has a slope to the skull and the ‘axis’ of the ear is therefore leaning such that the upper part is more outward than the inner part – there is no surgical solution to correct this. Some patients who have ear pinning surgery remain unhappy with the appearance of the ears after surgery even when the ears are within the ‘normal’ appearance.
Further information
BAPRAS information on prominent ear correction – click here